Care home ‘crisis’ as funding cuts loom
Exclusive: care homes in many parts of the United Kingdom are facing a grim combination of funding cuts and declining standards, according to figures obtained by Channel 4 News.

Channel 4 News has learned that funding of medical and nursing services for care home residents is set to fall by up to 11 per cent this financial year.
As care homes also face local authority cuts of between 20 and 30 per cent in accommodation funding and operators like Southern Cross suffer from the recession, the cuts could see some operators struggling to provide safe, high quality care or even to remain open, forcing some residents into expensive emergency hospital care.
Grave concerns have already been raised over the quality of some care homes.
Last week the Care Quality Commission closed 34 sub-standard homes as it brought in new regulations, and tomorrow an independent report is due which is expected to criticise Parkside House Nursing Home, in Northampton, over the deaths of five elderly residents.
The figures on funding were obtained by a Freedom of Information Act request from the GPs’ magazine, Pulse, and shared with Channel 4 News.
Problem is acute now
The Government has announced a commission into the funding of long-term care for the elderly but that will take some time to report and the problem is becoming acute now, writes Channel 4 News Social Affairs Correspondent Victoria Macdonald.
Not only are Primary Care Trusts cutting back but local authorities are contemplating 25 per cent cuts in funding. That is likely to mean more pressure on care homes and their residents and for the 25 per cent who pay for their own care, it could result in higher fees.
Age UK also warns that the cuts predicted in the Comprehensive Spending Review could mean an additional funding gap of £2.2 billion over the next four years.
That would mean that councils will only be able to help one in four of the older people who current receive home-based care and support.
And on top of all this, is the fact the ageing population is growing and by the time they go into care they have multiple and complex needs.
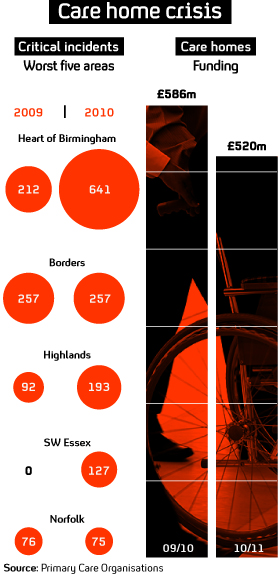
Last year, funding for medical and nursing services for care homes was £586m, from the primary care organisations across England, Scotland and Northern Ireland which responded to the FoI. For this financial year, 2010-2011, it fell by 11 per cent to £520m. More than eighty organisations provided data on funding.
Two organisations declined to comment in detail on their funding levels this year.
With their data removed, the figures stand at £565m last year, down to £520m this year – an overall fall of 8 per cent.
A Department of Health spokesman told Channel 4 News: “Care homes residents are entitled, as are all citizens, to the full range of NHS services, free at point of delivery. We expect the NHS locally to ensure that residents get the health services they need.
“The NHS has actually increased funding to meet the costs of a nurse that’s needed in a care home. It is the responsibility of care homes to negotiate with primary care trusts over local contracts for the provision of a continuing healthcare package for those assessed as eligible for NHS-funded continuing healthcare.
“The NHS White Paper proposals to make GPs responsible for commissioning decisions will help integrate health and social care. In addition, the Health Secretary today announced that around 35,000 people will be helped this financial year to settle back in their homes after a spell in hospital.”
Total crisis
Age UK‘s Director of Policy and Public Affairs, Andrew Harrop, told Channel 4 News: “These findings reinforce the impression we already have that our care system is in total crisis.
“A major spending cut in the next few years will make this situation hugely worse and unfortunately many older people will die as a result.”
Other figures obtained through the Freedom of Information process show that there was a leap in the number of “critical” or “serious untoward” incidents reported by care homes to over the last year, by 80 per cent.
The Editor of Pulse magazine, Richard Hoey, said: “It’s hard to see how funding cuts are going to improve this situation, and the worry has to be that they will further fuel the rising numbers of serious safety incidents.”
In 2008-2009, there were 864 incidents. In 2009-2010 there were 1,590.
Areas
Our graphic shows the funding drop and the different levels of reported critical incidents across the country – which do all have different numbers of elderly people in their communities.
Heart of Birmingham reported 641 accidents last year – including all commissioned beds – while Norfolk saw its figures remain steady, with 76 critical incidents investigated last year, and 75 this year.
Extreme concerns
Stephen Burke, Chief Executive of Counsel and Care, said: “We are extremely concerned to hear of this report…We hope further clarification can be given on the specific reasons why this huge jump has occurred.
“The findings add further fuel to our calls for the commission on funding of care and support to consider how to improve the quality of care in addition to focusing on how the care system will be funded in the future.
“They also show how urgent action is needed now to make sure that older people are not put at risk and can access the good quality care they deserve.”
Why the problem?
The rise in the number of incidents could be linked to a number of factors, experts said, from long term funding reductions leading to fewer staff on duty, to a stricter focus on care homes by regulatory bodies causing the care homes themselves to report incidents more diligently.
Judy Downing, chair of the Relatives and Residents Association, said staff turnover could be a factor.
Around 40 per cent of new recruits to care homes leave within one year.
“Staff turnover is a huge concern in care homes and we would like to see all staff have some training, particularly in dementia care, as a basic minimum.”
Age UK’s Andrew Harrop said: “We know the NHS and local government are severely underfunding care homes making it almost impossible for some operators to provide safe, good quality care. There is very likely to be a connection.”
'Shocked' at care home staff
Pamela Wells tells Channel 4 News about the "horrendous" treatment of her husband.
For some very ill patients, their places in care homes are fully funded by the NHS under its continuing care programme.
For Stephen Johnson’s brother Rod, this ought to have been the case after he had a major stroke in his early fifties and moved to a home from hospital.
But his local organisation turned him down for funding more than five times.
“I was banging my head against a wall,” he said. “Aneurin Bevan would be turning in his grave. It should be so simple.”
His family funded his brother’s care before his death in 2008. A few months after his death, Mr Johnson eventually received the £51,000 back from the NHS after his Continuing Care Campaign.
Complaints
A separate inquiry by Pulse magazine also found that the Care Quality Commission (CQC) received more than 69,000 complaints in the last five years about care homes – including 400 complaints of suspected sexual abuse.
There could have been even more complaints as, from April 2008, people were directed towards the providers themselves rather than the CQC with concerns.
There were more than 8,000 complaints about staff attitude and competence between 2004 and 2009. Some 4,626 complaints were registered regarding poor staff attitude, and 4,760 about staff competence or skills.
Richard Hoey, editor of Pulse, said: “Care homes have been backwaters of our health service for far too long, and on this evidence their residents seem to be viewed as soft targets for cuts…
“We have to work out ways that the NHS can look after these patients properly without it costing the earth, because we’re going to see major increases in their numbers over the coming years.”
The shocking figures come the week after the CQC revealed it closed 34 care homes and eight agencies providing care in peoples’ homes in the last 12 months.
The regulator stressed that the majority of the UK’s 24,000 care homes provide good care, but in a small number of cases risks to people’s health and welfare meant the only option was closure.
In the same period, another 51 services – representing 39 care homes – closed voluntarily after CQC rated them as “poor”.
The closures were ahead of the introduction of tougher new regulation for care homes, which came into force on 1 October.
-
Latest news
-
How drug gangs operate in Europe’s most dangerous city11m

-
Debate: Should there be an election in Scotland?6m

-
How Yousaf resignation could spell end of SNP dominance in Scotland3m

-
Rwanda effect on asylum seeker numbers ‘doubtful’, says Irish MEP4m

-
How is the UK’s Rwanda asylum plan impacting Ireland?8m

-




